Designing freestanding emergency departments for performance and adaptability
Emily Karbo, DNP, RN, EDAC, Associate AIA
Andy Collignon, AIA, JD, NREMT
Freestanding emergency departments (FSEDs) are an increasingly important part of the modern healthcare landscape.
As patient demand rises and access challenges grow, health systems are looking beyond hospital campuses to deliver emergency care closer to where people live. Typically located in rural or high-growth areas where access to hospital-based emergency care may be limited, FSEDs provide 24/7 emergency care outside of a hospital setting.
These facilities are equipped with imaging, laboratory services and staffed by at least one board-certified emergency physician, similar to a hospital-based emergency department, but improve access, reduce travel times and relieve demand on centralized emergency departments by bringing emergency services closer to growing and geographically dispersed populations. The number of FSEDs increased by 75% between 2005 and 2019, and according to Becker’s Hospital Review, cases in U.S. emergency departments are projected to increase by 8% between 2025 and 2035, driven by an aging population, limited access to primary care and continued population growth.
Strategic siting for performance, not just footprint
Location is a critical factor in FSED planning. These facilities are often built in suburban growth corridors or communities to expand access to emergency care at a closer proximity than the nearest hospital.
Unlike large hospital emergency departments, freestanding facilities must be lean and self-contained. Flexible exam rooms, adaptable treatment areas and efficient circulation are essential for managing fluctuating patient volumes to maximize the value of the space within a limited footprint.
Successful FSEDs require more than just the right location. Their design must support high-pressure clinical environments while remaining efficient and adaptable. Thoughtfully designed facilities typically include strategic configurations of exam rooms, trauma and resuscitation spaces, imaging and point-of-care laboratory services. These elements allow clinicians to treat a wide range of emergencies in a compact setting outside of a hospital.
“Our goal is to create a dynamic environment that performs under pressure,” said Emily Karbo, ESa’s clinical operations and design specialist. “By understanding how clinicians work and how patient needs and acuity vary, we design FSEDs that remain efficient, flexible and adaptable over time.”
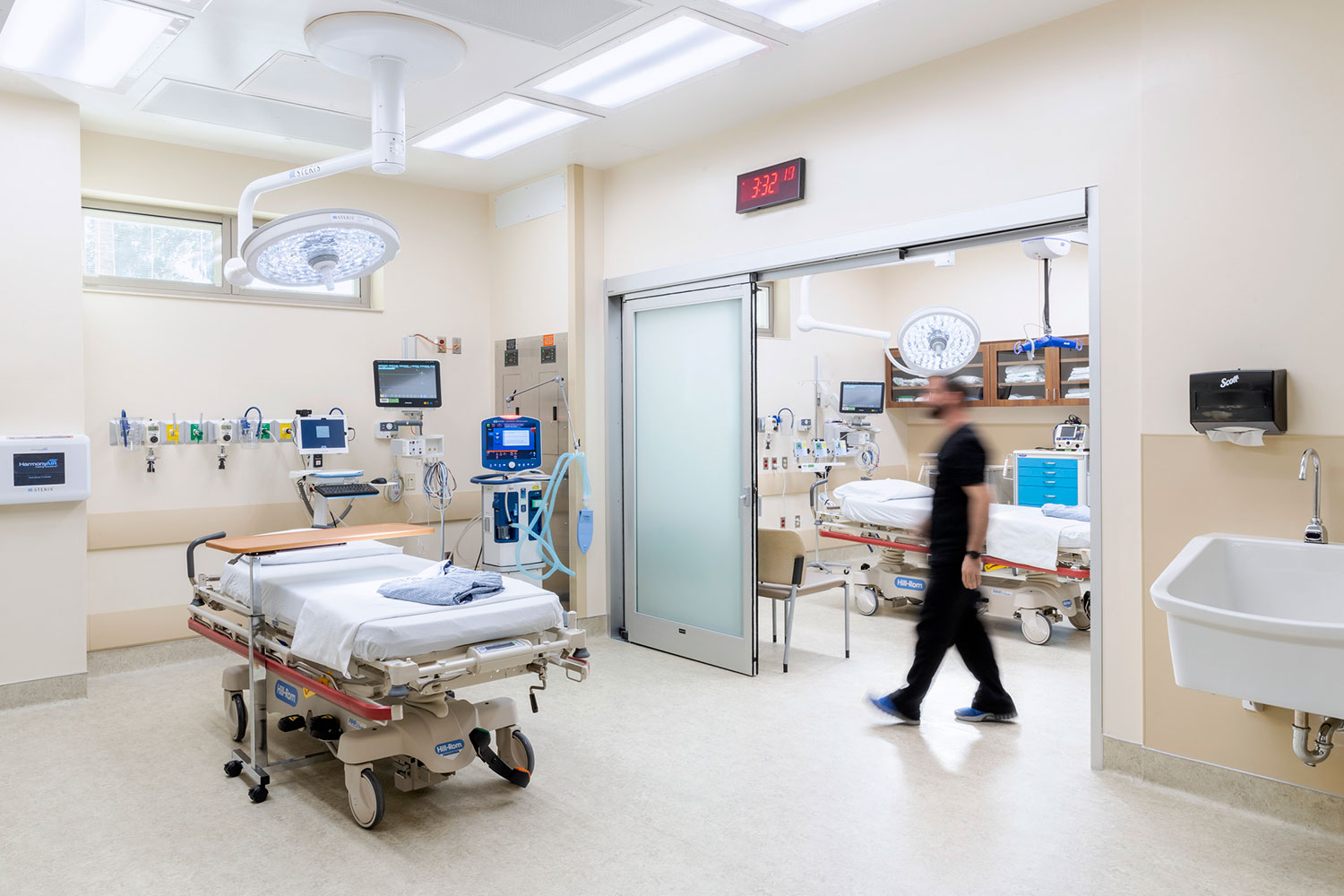
Provider and patient benefits by design
Thoughtful design improves safety and operational performance for both patients and clinicians. Clear visibility of entry points from staff work- stations help improve safety. Defined pathways also allow emergency teams to move quickly during critical situations.
Staff work zones are typically organized to maximize visibility and oversight across treatment spaces, allowing providers to monitor patients efficiently while supporting lean staffing models common in freestanding facilities. Backed by operational data, benchmarking and health system planning, design decisions ensure seamless escalation of care when needed.
“When the space is designed around how clinicians actually deliver care, it allows them to focus on patients instead of workarounds,” Karbo said. “That level of design support directly impacts safety, efficiency and the health of our communities.”
Design measures also influence the patient experience. Integrating wellness-driven principles such as natural daylight, intuitive wayfinding and calming color palettes is key for reducing stress for patients and families.
Where clinical insight meets long-term planning
FSEDs are no longer simply overflow solutions for crowded hospitals. They are an important piece of an organization’s overall strategy to improve access to medical services for the population by providing access to timely emergency care. Typically, between 3 and 6% of patients visiting an FSED will eventually be transferred to an acute care facility for admission.
At ESa, designing effective freestanding emergency departments begins with collaboration. Our team works closely with clinicians and health system leaders to understand both staff and patient needs, operational goals and community context before design begins. This approach ensures that facilities support both clinical workflows and long-term strategic objectives.
Successful design anticipates future growth and evolving patient acuity. When facilities are planned with adaptability in mind, they become durable assets within modern health systems. And when designed with purpose, they are built to perform for decades to come.
See how ESa approaches design with purpose and why longevity is never an accident.